In 2022, the Egyptian Medical Syndicate released a shocking report, finding that over 10,000 Egyptian doctors resigned from positions in government hospitals during the prior three years. In the same year, MP Hazem El Gendy told his colleagues during a parliamentary session that the situation was actually much more dire, estimating that 110,000 doctors—or just about half of all doctors in the country—had left since 2019.
While the strain of the COVID-19 pandemic was certainly a precipitating factor in this unprecedented brain drain, as it has been in health systems around the world, El Gendy pointed to “low wages, as well as the low medical capacity and supplies inside public hospitals, despite the increase in budgets allocated to the medical sector and its tangible development – in addition to seeking better opportunities for scientific research and the lack of legal protection for doctors in the exercise of their profession.” The flight of these trained professionals is especially worrisome in a country that, in 2018, already had less than half the global average of physicians per 1,000 inhabitants and about half the average of the Middle East and North Africa (MENA) region as a whole (1.6 globally, 1.4 in MENA, and 0.7 in Egypt).
On the other hand, the COVID-19 pandemic precipitated a large influx of foreign-born health workers into many of the Gulf states, especially Saudi Arabia. Despite efforts in the region to increase rates of domestic health personnel, half of the physicians who work for the Saudi Ministry of Health and more than one-third (37 percent) of nurses are migrants. These professionals cited factors like higher salaries, paid vacations, free flights to their home countries, easier job entry requirements than in western nations, shared religion, and the country’s better health facilities and technologies.
The population of the Arab world was just over 456 million people in 2021, including nationals and expatriates. Today, youth and young adults (those between the ages of 0-24), who are usually relatively healthy populations, make up the majority of the region. However, as these populations age, their health needs will increase, and the traditional model in the region of children living with and caring for their aging parents is changing as young adults are more likely to move to urban centers and live in individual apartments or condos, and as women typically expected to handle caregiving duties are themselves moving or pursuing employment instead. Further, although population growth rates in the region have declined, it is estimated that the population throughout the Middle East will double in size by 2050. Varying health workforce challenges throughout the distinct countries of the region means that the health care systems may be unable to meet population needs. This could become a significant unneeded and unwanted threat to the region’s social, economic, and political stability.
Health Workforce Migration
The health care systems, needs, and outcomes in countries of the Arab world are as varied as the countries themselves. Their pre-existing conditions, especially those affected by conflict, political instability, poverty, and corruption, play a large part in a health system’s ability to function, particularly as it relates to health workforce migration. In 2023, the World Health Organization (WHO) had four Arab nations on its list of countries that needed specific health workforce support and safeguards: Djibouti, Somalia, Sudan, and Yemen. Not surprisingly, all are countries variably affected by conflict and violence. WHO guidelines for these and other nations facing health workforce challenges are clear: they should not only be prioritized for health system and personnel support, but their health workers should not be actively recruited internationally.
In the Gaza Strip, the Israeli siege has led to the inability of physicians to practice medicine with proper equipment or livable wages. There is also the risk of death due to bombardment, as happened to two doctors who were killed by Israeli bombing in 2021. Both were specialists, which are badly needed in the besieged territory. Thus, it is no surprise that many physicians feel compelled to leave Gaza for secure job opportunities abroad. In 2019, the emigration of a heart surgeon led to the shuttering of a hospital’s entire Department of Cardiac Surgery. Hospital staff called his departure a “catastrophe.”
Many physicians feel compelled to leave for secure job opportunities abroad.
Yemen has seen similar trends, especially toward the beginning of the current war in 2014. Health professionals who themselves were suffering trauma were unable to fulfill their duties due to lack of medicines and supplies. Patients who managed to make it to a health facility could not afford to pay for services. In November 2022, only 51 percent of Yemen’s health facilities were still functioning, despite the need of nearly 22 million people for critical health services. In Syria, a concentration of bombing attacks on medical facilities led to the death of hundreds of health workers. Even if one survived, other threats included risk of kidnapping, torture, and imprisonment. Approximately 70 percent of the country’s health care workers fled, leaving some areas completely devoid of health care facilities. Medical schools were also disrupted, leaving massive gaps in a trained workforce. These conflict-affected countries can hardly recruit medical personnel from abroad, with the exception of those working with humanitarian agencies on short-term missions.
Of course, it does not require overt political violence to lead to health worker emigration. Lebanon had long been known as a medical hub in the region and was a popular destination for medical tourism. Medical tourism generated $1.2 billion in growth for the country in 2014. But for decades, Lebanon has been facing political and economic challenges that have slowly and finally worn away the country’s health sector workforce. This has quickened in recent years, especially since the explosion of the Port of Beirut in 2020. Several health care facilities were destroyed in the blast, and many health workers were injured or killed. As the governance crisis of the country came to a head, there has been increased emigration of the country’s doctors and nurses, especially as the value of the Lebanese pound has continued to plummet. One doctor recounted that his current salary is worth less than 50 cents per hour: “If my country cannot provide me with a decent salary after 13 years of study and work, what’s the point?”
Saudi Arabia is estimated to need at least 20,000 more doctors by 2030 to ensure adequate staffing of facilities.
While the Gulf countries are better situated to manage population health needs due to their wealth, they are also predicted to have a greater demand for health care than any other region in the world—a 240 percent increase over the next two decades. Saudi Arabia is estimated to need at least 20,000 more doctors by 2030 to ensure adequate staffing of facilities. The country has been heavily reliant on migrant health care workers from around the world, although it has invested in efforts to train and maintain Saudi nationals as health professionals. Ironically, many locally trained medical staff migrate to Western countries for better training and employment opportunities. In 2022, the country engaged in a Health Sector Transformation Program as part of Vision 2030 that entails encouraging Saudi nationals to pursue careers in the health sector. Other Gulf nations are also attempting to decrease reliance on an expatriate health workforce, but as these efforts are rather nascent, their success remains to be seen.
Reviving the Region’s Health Workforce
It is clear that throughout the region, reform in the training, recruitment, and retention of medical professionals is desperately needed. While not all Arab countries face the same level of shortages, there is not a country in the region that is adequately producing and then employing enough citizens as medical workers for their growing populations and their distinct needs. Some have even called for international actors, especially the United States, to rebuild influence in the region not through defense or energy agreements, but investments in health.
One often posed solution is to build more medical and nursing colleges and create incentives for nationals to pursue medical careers. While many countries once boasted robust and vibrant health and education systems—like the aforementioned Lebanon, Iraq, and Tunisia, among others—decades of conflict, corruption, and other struggles have reversed the trend, leading to flight of professionals in many sectors. However, the loss of health professionals is among the most urgent. There have been some efforts to invest in health infrastructure; for example, Egypt established two new government medical colleges, Al-Arish and al-Wadi al-Jadid. Jordan, which has seen high unemployment rates among medical graduates, has slowed enrollment in medical schools at public universities while granting licenses for private universities to build their own medical colleges. Saudi Arabia is working to increase its number of medical schools from 5 to 37.
Yet some argue that the region is actually training enough doctors, but too many graduates want to leave immediately upon completing their training due to poor conditions in their home countries. Egypt, where the shortages in personnel are very stark, actually trains many doctors per its population, but the newly minted professionals face exceedingly low salaries that are not commensurate with the competitive nature of medical school spots and the amount of time and energy needed to successfully finish—for example, around $200 per month in Egypt. In Tunisia, an experienced specialist might make just $15,000 per year—the equivalent of a monthly salary for the same job in the Gulf. Medical graduates wish to escape crowded, under resourced, and unstable working conditions for the opportunity to work in higher income countries.
Too many doctors want to leave immediately upon completing their training due to poor conditions in their home countries.
Aside from the loss of the trained physicians, the loss of capital is meaningful on a larger scale. In Sudan, for example, workers often train in the country but then go elsewhere for work—one expert estimated that the country spends $24 million per year training doctors who then leave the country, and that there were probably as many Sudanese doctors in Saudi Arabia as there were in Sudan. This illustrates a fundamental issue that requires policy intervention: creating incentives for locals to not only train in health professions but stay in the country upon completing their education. While it is not workable to merely wait for political resolution or economic improvement before making meaningful investments in a nation’s health workforce, it is clear that low wages and inadequate conditions are a major factor pushing young, ambitious, and educated people out of the countries that need their skills the most. Governments must find ways to improve conditions, boost morale, and provide job and wage security if they want to be able to meet the needs of their growing populations—let alone plan for the potential unknown challenges ahead.
Empowering women throughout the medical field is an important way to boost local health capacity while providing needed educational and employment opportunities for women. The low number of female physicians and specialists in the region is also detrimental for patients, as some women, by choice or through familial pressure, might avoid seeking care or receiving treatment from a male physician. Reforming laws that bar women from certain training or employment opportunities or prevent their freedom of movement would be a vital first step in such an initiative, followed by policies that change cultural norms around women in the workplace and offer them support through policies like maternal leave. Fortunately, the gender gap in the health sector has been decreasing as women enter more auxiliary roles in medicine, but their economic or political power has not followed suit.
As was the trend throughout the COVID-19 pandemic, there has been a significant rise in deployment of telehealth services around the world. Some have posited this as a potential solution to health workforce issues, including in MENA. Internet access and smartphone utilization have significantly increased in the region in recent years—as is, the telehealth market of the region is set to grow by 26.3 percent from 2022 to 2030. Telehealth can help overcome some issues of access, allowing people to reach a doctor, nurse, or pharmacist via phone, video, or chat and receive care for many ailments. In theory, this would also free up local health capacity for patients who require advanced or long-term care. However, overt reliance on telehealth still poses a host of accessibility issues for those in areas without sufficient internet access or without the needed technology. Further, telehealth does not fix the issue of flight of trained professionals and does not replace having a responsive and well-funded health system.
The countries of the Arab world are not alone in facing struggles training and retaining qualified medical personnel. WHO estimates a global shortfall of 10 million health workers by 2030, concentrated in low- and lower-middle income countries. Dependence on foreign-born medical professionals is not sustainable, especially in a world of potential shocks to travel, like the COVID-19 pandemic, and is also potentially unethical if actively recruiting medical professionals from countries that need them. Further, the fragile countries of the region have little hope of recruiting health professionals from abroad who would stay. Deterioration in health systems will undoubtedly ripple out into other sectors, like education, economics, and politics. To ensure growth, stability, and opportunity for their citizens, Arab countries must recognize that a stable health system staffed by well-trained workers is not a luxury, but a necessity.
The views expressed in this publication are the author’s own and do not necessarily reflect the position of Arab Center Washington DC, its staff, or its Board of Directors.
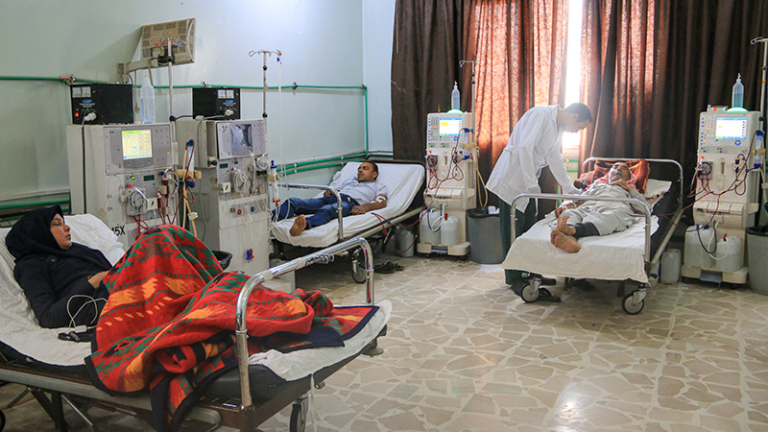
Featured image credit: Shutterstock/Mohammad Bash

